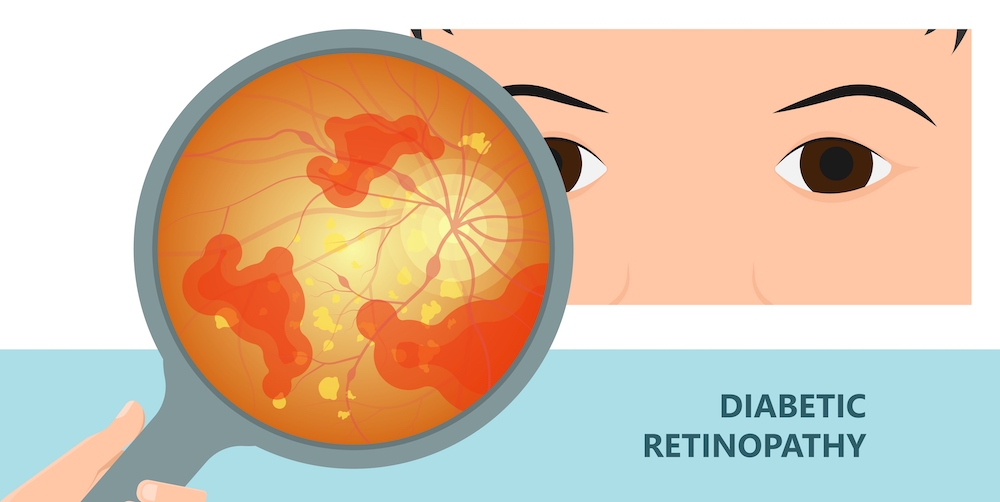
Diabetic retinopathy can cause blindness in adults and vision loss in people with diabetes. Unfortunately, it can easily go unnoticed in its early stages. Regular comprehensive dilated eye exams—at least once a year—can help detect it early and prevent further complications. Maintaining control of diabetes and addressing early symptoms are crucial to preventing diabetic retinopathy.
What Is Diabetic Retinopathy?
Diabetic retinopathy is a condition that involves damage to the retina's blood vessels, the eye's crucial component for detecting light.
To avoid potential complications, those with diabetes should undergo a thorough eye exam with dilated pupils annually. The initial stages of diabetic retinopathy may not show any signs. Yet, early detection can play a crucial role in preserving vision.
Stages of Diabetic Retinopathy
Nonproliferative retinopathy – This is the initial stage of diabetic retinopathy. It is where blood vessels in the retina become dilated and prone to leakage. The situation can result in macular edema, leading to a mild decline in vision. Proper treatment can decrease this swelling. In some cases, the lack of sufficient blood flow to the retina may also affect the health of the nerve cells, causing further vision impairments.
Proliferative retinopathy – This is the advanced stage of diabetic retinopathy. It occurs when new blood vessels develop abnormally on the retinal surface. These blood vessels can become fragile and leak into the vitreous, leading to significant vision loss. Swift treatment is necessary to prevent further complications at this stage.
Symptoms
Diabetic retinopathy often advances silently, with symptoms emerging only when the condition progresses. As it advances, you may experience the following symptoms:
Blurred or double vision
Rings or flashing lights
Blank spots in your vision
Floating or dark spots in your vision
Pain or pressure in one or both eyes
In some cases, diabetic retinopathy may cause macular edema. This complication occurs when the central part of the retina swells from leaking fluid, leading to blurred vision. Also, new vessels growing on the retinal surface and bleeding into the eye can decrease vision.
Complications
Diabetic retinopathy can lead to numerous complications, such as vitreous hemorrhage, if left untreated. That occurs when blood vessels in the eye bleed into the vitreous that fills the eye. In mild cases, you may experience floaters, but more severe cases can result in vision loss as the blood in the vitreous blocks light from entering the eye.
But if the retina remains undamaged, the bleeding in the vitreous can resolve independently. In some cases, diabetic retinopathy can result in a detached retina. This is a condition where scar tissue pulls the retina away from the back of the eye. It causes flashes, floating spots in your field of vision, and severe vision loss.
A detached retina can lead to total vision loss if not treated. Additionally, the formation of new blood vessels can block the normal flow of fluid in the eye, leading to glaucoma. It can also increase eye pressure, potentially causing optic nerve damage and vision loss.
Conclusion
Taking steps to prevent diabetic retinopathy from developing or becoming more severe is essential. It starts with regular eye exams. Early detection and proper management of diabetes can help minimize the risk of developing this condition.
For more on diabetic retinopathy, visit Dr. Richard E. Hults & Associates at our Elyria, Akron, Fairview Park, or Canton, Ohio, offices. Visit our website to schedule an appointment today.
















